It’s one year since I had a home birth. Actually, a Home Birth after a Caesarean Section, or HBAC as it’s known, with my second child. I thought it would be the perfect time to reflect on that birth and write up for home birth story for you.
Home birth story
My previous birth – a category 1 emergency c-section
My eldest was born at 42+1 by a category one emergency section in December 2011 after a classic failed induction and cascade of interventions.
You can read that birth story here.
It involved my waters being artificially broken, syntocinon, two doses of diamorphine, gas and air and eventually an epidural. I was also catheterised twice, then given a general anaesthetic for the surgery.
My son was Occiput Posterior (OP), aka back to back, and syntocinon was making me over-contract and the baby’s heart rate decelerate.
They took blood samples and his oxygen levels seemed to be plummeting. They said, ‘We’ve got to get this baby out now’ and then bizarrely ‘do you trust us to safely deliver your baby?’. WTF, what else am I going to do?!!
Neither me or my partner saw our baby born. I suffered birth trauma and felt terrible physically and emotionally. Fortunately, the baby was great with apgars of 9, 9.
As you will know if you are a mother, every birthday you remember and reflect upon your child’s birth. For me, my son’s birth wasn’t something I was proud of, it made me feel sad, I felt like a failure (even though rationally I knew that was not the case).

My HBAC home birth story
It’s my daughter’s 1st birthday tomorrow and finally, the birth reflection is good! I’m smiling thinking about it. I have a warm feeling in the pit of my stomach.
I had no drugs so I remember it clearly – unlike my first birth.
I’m proud of the way I handled myself during the birth and I’m still confident the decisions I made were the right ones for us.
I feel strong and empowered when I think about it. It changed me, as each birth does.
This is why birth is so important. It impacts women and families in a myriad of ways forever. I challenge you to think of anything more important, that makes more of an impact in so many ways.
That is why I wholeheartedly support the recent news of the upcoming changes to maternity care borne from the NHS Maternity Review.
I had a birth that was different to what is ‘the norm’ in England. Indeed, it was against what is ‘medically’ recommended in terms of having a HBAC instead of a Vaginal birth after a C-section (VBAC) in a hospital.
I had done a lot of research and based on that research as well as my own gut instinct, I knew a home birth was the right choice for us and therefore the safest option.
I had to really fight for my right to my own choices through informed consent. I will do another post on tips for achieving a HBAC but for now I’ll share my home birth story.
Warning, it’s a long one – because my labour was!
The start of my home birth story – Monday 23rd

Monday 23rd February 2015 was my due date based on when I felt I might have ovulated. I was 41 weeks based on my scan dates.
My doula came to pick me up and we both went to my chiropractor appointment with my three year old.
My chiropractor (Zoe Freedman Fossey in Blaydon for those in the North East of England) specialises in pregnancy and babies.
I had been working with her for a while to resolve some issues with my pelvis being misaligned and my piriformis muscle being too tight which she felt contributed to my long, stalled posterior labour with my first birth, and eventual emergency c section.
My chiropractor was pleased with my progress, she felt the exercises I had been doing daily to loosen my piriformis had made a big difference, she was confident I shouldn’t have the same issues as last time.
The baby was Left Occiput Anterior (LOA) so perfectly positioned which pleased me after my last posterior labour.
She did some acupressure points that are supposed to help induce labour. She showed my doula some pressure points that could help if labour stalled again this time.
We went home and I spoke to my mam on Skype. I felt a bit ‘chewed’ and was having more crampy braxton hicks.
I continued to press the acupressure points the chiropractor had shown me. Looking back I think this is when my early labour began but the contractions weren’t regular enough to make me time them yet.
Home birth story – Tuesday 24th
Contractions happened more on Tuesday and by the evening were enough to make me start timing them out of curiosity.
They were lasting a minute and painful but not getting closer together, they were usually around ten minutes apart. Sometimes less, sometimes more.
I had my ‘bloody show’ in the night and this continued over the next few days. It was hard to sleep Tuesday night, from a mixture of excitement and discomfort.
The contractions were more painful when I laid down but I knew it was important to try and rest in these early stages so I played natal hypnotherapy which was always great at putting me to sleep!
Home birth story – Wednesday 25th

During the day my partner stayed off work and my son was in nursery for the day in anticipation of labour ramping up, but the contractions slowed down a little.
They continued through the day but not as frequent as the night which was very disappointing.
We had a calm and relaxed day, watched some shows and enjoyed the time together. I just breathed through the contractions when they came.
I actually watched a really great birthing show and was chatting with some of the women from it on a home birth Facebook group and I found that inspiring.
Through the night the contractions increased again just as before. It was a tiring night but when the morning came they slowed back down again.
Home birth story – Thursday 26th
My midwife called me to tell me the ‘Ward Manager’ wanted to meet with me to discuss my post 42 week plans.
I had already declined sweeps and induction and was to go in for my first monitoring session at 42 weeks (Monday).
I told her I didn’t think it was necessary as I thought I was in slow labour. I contracted a few times on the phone to her and had to stop talking.
Then later in the day my midwife turned up unannounced to check me over. I think they were anxious about me, as I was going against recommendations to birth at home so were taking every precaution.
All was well, the baby was 3/5ths engaged. It was reassuring to know we were both doing so well.
My midwife informed me she was on call that night for my home birth. I was so pleased to hear this as I was hoping she would be the one to attend as she knew my wishes in depth.
The midwife recommended to start using the tens machine but it was annoying me at this stage.
I was starting to feel a little disheartened at the second day of labour slowing down so my doula (who is now a midwife herself) offered to pop over for a pep talk.
This helped me get into a more positive head space again. While people were with me (the midwives, the doula) the contractions slowed right down almost to a stop.
It was suggested perhaps this was because I was too tired from the past two nights of labouring and I should nap which I did.
Home birth story – active labour
They were right. When I woke up from the nap, the contractions started coming more regularly.
This continued and by tea time I was starting to become more confident that I was moving towards established labour.
I continued to use my hypnobirthing breathing to manage the contractions. I started to use the tens machine which was now really helpful.
My partner made dinner and I managed a few bites of chicken and some chips.
We arranged child care for that night and my son went to his grandad’s at about 7pm.
While my partner got our son ready to go to his dad’s I finished setting up the birth room which was a great little project to do at this point in labour.

I had printed out a lot of birth affirmation posters to put on the walls so I started to put these up, reading them and being inspired by them as I went.
I put candles around (I recommend battery ones which are safer and less hassle than real ones) and tidied the room to how I wanted it.
We put relaxation music on and turned the lights off to candle light.
I set up a base at a tall chest of drawers with my water, coconut water and phone etc on it. I took some paracetamol.
I found the drawers were just the right height to allow me to lean on them while standing with my arms over the top, resting my head on my arms to breathe through the contractions.

I couldn’t sit down or lie down as the contractions became much more painful when I tried. I stood and walked for hours.
That chest of drawers was an unanticipated godsend. I hadn’t factored it into my plans but it turned out to be a huge tool in my labour. Funny how that can happen.
The tens machine was also very helpful. When I forgot to turn off the intermittent setting between contractions and couldn’t feel the benefit of the pulse setting during a contraction, I really noticed the difference.
I would thoroughly recommend a tens machine (amazon affiliate link) for labour. I was surprised how much it helped. I had it for my first labour and hadn’t even used it. I could kick myself for assuming it wouldn’t be helpful.
Natal hypnotherapy in practice at a home birth
I had practiced natal hypnotherapy for months before my due date and I’m sure this helped me maintain the right frame of mind on the day.
I didn’t listen to the CDs (amazon affiliate link) during established labour as I had planned, I just didn’t feel like it. Instead I listened to general relaxation music that we had got from YouTube.
I also didn’t use the visualisations I had practiced. Instead, I gave myself and my daughter pep talks in my head, I thought about how we were working as a team to do it together and thought about all the other women who had done this before me, and were doing this with me. I found my little motivational chats in my head more helpful than the visualisations.
The slow deep breathing was most helpful though. On each contraction I would breathe in deeply through my nose, deep down to my baby and then out slowly again through my mouth. I managed all my contractions doing this.
I didn’t even consider gas and air. The contractions were nowhere near as painful as my previous syntocinon labour, not even in the same league. They were totally manageable.
I beasted out those contractions like a queen! On a whole I think this was down to all the natal hypnotherapy practice and other mental preparations I had made in the months leading to the birth. Unlike my first birth, I was ready for this.
When to call the midwives for a home birth?
I kept chatting to the doula about when to call the midwives. My midwife had suggested to call her when the contractions were 8 minutes apart, which they had been since early afternoon.
I felt that was much too early though. I didn’t want the midwives there too early as I was anxious about being put on timescales and increasing the risk of transfer to hospital – especially considering their anxiety about me going against medical advice.
The contractions were now about 3-4 minutes apart (from around 8pm). At some points I was throwing up – a terrible combination of chicken and coconut water that will live with me forever!
Waters breaking at a home birth
Then at about 10.20pm I felt a strange cracking pop during a particularly intense contraction, it was like joints rubbing together or something like that, I said ‘what the hell was that’ then felt my waters trickle out and realised what it was.
I didn’t expect waters going to feel like that. I thought something had snapped.
You know when people say ‘oh I didn’t know whether my waters had gone or I had peed’? Well for me it was more, ‘I don’t know if my waters have gone or I’ve broken my spine’. Then I went to the loo and threw up again.
Things became more intense from then on and contractions were every 1-2 minutes, I knew it was time to call the midwives (which we did at 11.10pm) and get in the birthing pool.

Home birth – birthing pool and transition
I had always thought the birthing pool would be amazing. I found swimming and being in water so soothing during my pregnancy so I thought it would be my saviour.
Unfortunately, I didn’t find it that great. It may partly have been down to the time in my labour that I got in.
I had clarity that I was in transition and said out loud ‘I feel panicky and like I can’t do this but I know I can its just transition’.
My issue was I really wanted to be upright, as ‘relaxed’ positions made the contractions more intense but by this point I had been standing for hours and at 41 and a half weeks pregnant, my legs were tired.
I also had to take the tens machine off to get in the pool which had been helping so much, and I missed it when it was gone but I could not find a comfortable position in the water.
I was mostly on my knees resting over the side but my legs and feet kept going numb from it.
I would alternate from this position to reclined backwards which I’m sure wasn’t optimal for gravity’s assistance.
Pushing stage at a home birth
Not long after getting in the pool I started to involuntarily push. My body was just bearing down naturally with the contractions and it felt good.
It took the midwives almost an hour and a half to arrive, given that I was pushing before they came there was a time that we thought I might have her in the pool before they got there.
I actually didn’t feel too worried about this though (my birth partners were). I thought if she came it would be fine but I did hope they would arrive soon.
Little did we know I would be pushing for 4.5 hours!
Home birth – final day Friday 27th

The midwives arrived 12.30am. I couldn’t have wished for better midwives. One was my antenatal midwife who had been my midwife for my son three years previously, as well as this time.
The other, it turned out is from my small home town. They later told my doula that some of the midwives were not keen to come to my birth because I was a HBAC (and probably seen as problematic given my complaints letters about poor home birth service provision and non evidence based policies).
My second midwife had volunteered to come. She had a home birth herself previously. I certainly benefitted from having someone who had actively volunteered to come to my birth and I’m pleased I didn’t get a midwife who wasn’t comfortable supporting me.
She was wonderful and the two midwives worked excellently together as a team. A real tribute to the NHS and the kind of care I wish every woman got on the NHS every time. They were very reassuring and calm.
The midwife I hadn’t met before always seemed to say the right thing to me at the right time. She was very encouraging. It was also great to see the community midwife that I had grown to know over the years at a birth. Whilst she had been perfectly proficient at the antenatal side, it was clear that this is where she excelled. You could see this was her life-blood and I felt grateful to have her by my side.
The midwives listened in with the Doppler regularly and it felt unobtrusive. As planned, I declined vaginal exams.
The midwives knew about this before they got to me as I had discussed my plans with my midwife in depth and she briefed the other midwife on the car ride to my house. They had also agreed my community midwife would lead on the birth with the new midwife taking notes and supporting which was a sound plan.
When they arrived they could see I was close to the end as I was pushing. They suggested I got out for a vaginal exam after one lot of contractions showed decelerations but I told them that I couldn’t lie down. I wasn’t pressured in the slightest.
At 1.05am they noted that the ‘red/blue line was visible in natal cleft’. Just after this I pushed the head partially out (a caput), however we learned the baby was posterior and badly positioned.
Home birth – coached pushing
At some point it had changed so not all the pushes were involuntarily and I was now being ‘coached’ by people in the room to push harder and longer etc.
This was something I had said I didn’t want in my birth plan and the only part of my birth I was not happy with, largely because it was the only time I felt I was listening to external voices and factors instead of my own internal voice.
I wonder whether it would have been different had I listened to my gut? Would I have rested a bit more at this stage and allowed the baby to get into a better position? Obviously I’ll never know, the midwives don’t think so anyway.
I’m just happy that I was at home as I have been told that if I was in the hospital forceps would have been pushed and I would have been under a lot of pressure from the staff.
I’m grateful my midwives were calm and supportive and didn’t suggest transfer. They actually reassured me constantly and joked about how they had never seen such a happy baby (stats wise) considering the position she had been in for so long.
Other midwives who came to do my postnatal check ups told me ‘oh I wouldn’t have let you push that long, I would have had you transferred’ reminding me how lucky I was to get the midwives I did (who knew not to use infuriating language like ‘let’ or ‘allow’ to a woman, let alone coerce her).
Home birth – stuck baby
I could feel the head was partially out. I could also feel how much it was over to one side and how much skin was still over it. I was thinking that there was no way that much skin could give without a terrible tear.
The midwives told me not to fear tearing. My doula later told me that she was fearful for how badly my perineum would tear from how it looked.
I was giving it my all pushing and I knew I wasn’t making good progress. She was well and truly stuck. I couldn’t get across that I wasn’t just saying ‘I can’t do this’. I rationally and pragmatically felt her position meant I couldn’t push her out by myself, she was being held back more than the power I had to push her out.
I worried that if I didn’t get her out soon she would get distressed and I would be transferred and ‘fail’ right at the end.
I can’t emphasise how much a c-section would have devastated me. Fortunately my baby’s stats on the Doppler remained reassuringly great.
I got out of the pool to try some different positions. Standing, squatting, leaning over the birthing ball etc but it didn’t help.
My doula fed me some honey and Haribos to see if the sugar would help me.
Home birth episiotomy
An episiotomy was suggested but we tried a bit longer and I asked for opinions.
My doula said ‘there is no way you are getting out of this with an intact perineum either way’ which is exactly what I had thought. I knew she was right, I needed to hear that. I consented to the episiotomy and am still happy with that decision.
I kind of wish I had done it earlier actually but at least I know we did everything we could. I think I can live with the decision to wait and cause more temporary damage to myself, than getting the episiotomy earlier and having to live with wondering whether I could have done it myself.
After they gave me the local anaesthetic they thought I might get her out without the episiotomy again but when I tried again and didn’t manage it they went ahead and did it. She just flew out, head and body all in that contraction at 3.18am. I really needed what turned out to be a half episiotomy.
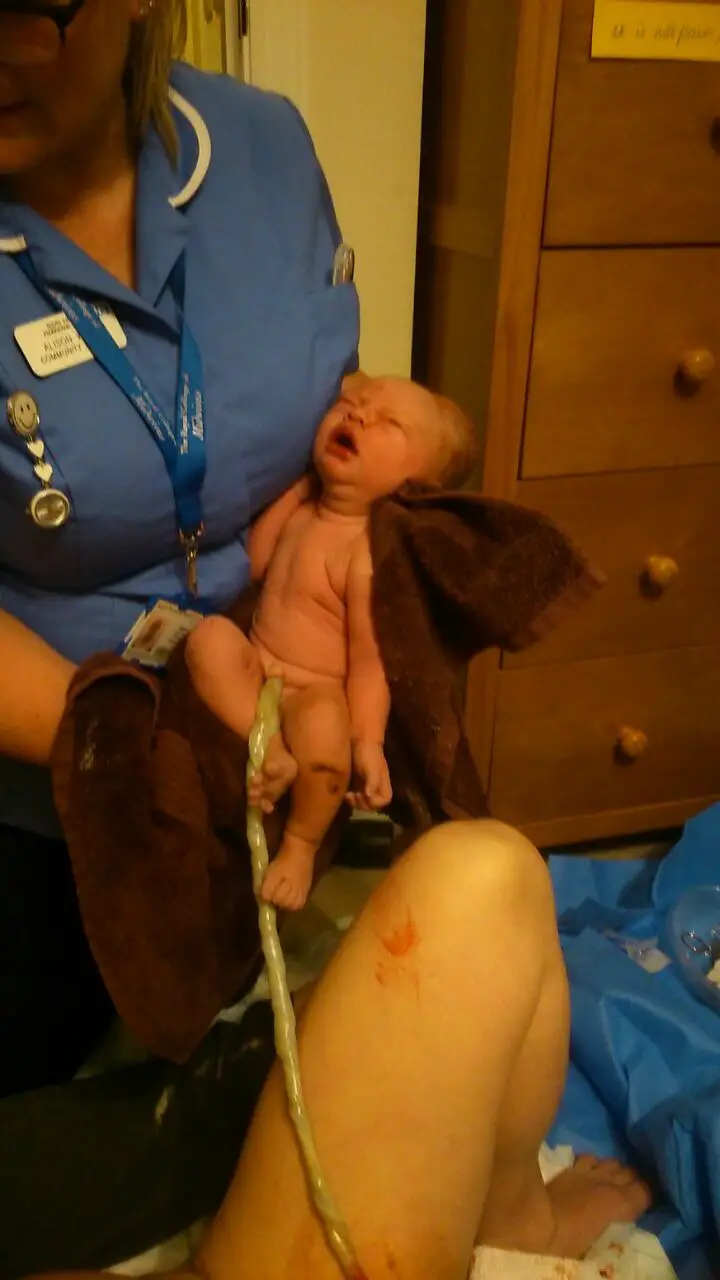
She was put straight on me – covered in blood and the meconium she passed on the way out. After all my active labouring I actually gave birth on my back but given that it was on my floor, laid in between my partner’s legs in his arms, it was actually kinda nice. Especially given he hadn’t seen our son be born.

I expected an immediate feeling of euphoria, relief, love and ecstasy etc but I actually just felt really awful from it all.
I wanted to pass out or throw up but to be fair to myself I was exhausted from pushing for hours.
Home birth – physiological third stage
We did delayed cord clamping until it stopped pulsating and a physiological 3rd stage. The placenta pretty much just fell out when I went to the toilet, no contractions or pushing.
My partner cut the cord. That is against our local hospital policy so that was really nice he was able to do that because we were at home too. I’m really pleased I did a natural 3rd stage.
Then I had my stitches in an armchair (which were fine) and everyone helped clear up.
Definitely buy a pump to drain the pool. We tried the ‘toilet flushing trick’ but it failed us and we wasted a lot of newborn cuddling time trying to sort that out!
I nursed the baby who we named Lena, a chubby 8lbs 5oz champion.
Everyone was gone by about 7am and we went to our own king sized cosy bed together. No awful hospital ward where your partner gets sent home and you are left alone exhausted and in pain.
Final reflections on my HBAC home birth story
I don’t have the words describe to you how different this labour was to my first. My first induced labour with syntocinon was the most painful thing I had ever experienced. There were times I genuinely felt the pain was so bad it might kill me. I was over-contracting and had no let-up from contractions in 17.5 hours before the emergency section. I did not feel in control or calm. I felt incredibly overwhelmed.
But at home in my own environment using the natal hypnotherapy it was so manageable, even without drugs. I felt totally in control – and powerful. I kind of enjoyed it in a way despite it being a challenge. The pushing stage was the hardest work I had ever done.
It was truly exhausting but at no time did I feel the pain was more than me. It has made me realise just how much your attitude, preparation and environment can affect your labour. I had read about it of course but I didn’t realise just how true it all was until going through it.
Despite the very long pushing stage (4.5 hours) with the head partially out (that left me with a nasty vulval hematoma) plus the episiotomy and stitches, it was still everything I had hoped for.
It was a really healing and empowering experience. Instead of feeling like a failure like last time, I feel strong and badass, reaffirmed – like I can do anything now! We got to see our baby be born this time – that was everything to us.
The healing was tough, I couldn’t sit for weeks but it was still much better than my category one emergency c-section recovery.
I had to be brave to go for the HBAC in the face of all the naysayers and at times I felt the battles with the NHS demoralising but I’m so pleased I trusted my gut and went for it.
When it came down to it, on the day, I had no doubts at all – something other home birthers told me they had found too.
I trusted myself and that was a great life lesson. I’d never birth in a hospital again! Home births rule!
Thank you
Thank you to everyone who offered me support and advice along the way, specifically the VBAC Support Group UK, Home Birth UK, Home Birth Chat Group UK and Home Birth North East on Facebook; my family, my friends, my doula and my midwives.
As is often the case other women were an intrinsic part of my success. When we hold each other up, there is nothing that we can’t achieve.
If you have enjoyed this HBAC birth story then I would love it if you followed me on Facebook, Twitter and Instagram so you don’t miss another.
You might also enjoy my other pregnancy and childbirth posts:
- My ultimate guide to pregnancy and childbirth
- Emergency c-section birth story
- How I overcame my birth trauma
- Placenta encapsulation – an honest experience
- 3 pieces of advice for women who are planning on having kids in the future…
- Breastfeeding a child with CMPA
If you have enjoyed this post or found it useful, here are some quick and easy ways that you can support Nomipalony or say thanks:
- Share this post with your friends
- Follow Nomipalony on Facebook, X, Instagram, Pinterest, YouTube or Tik Tok
- Pop over to my Amazon Storefront to see what products I have been buying and loving from there recently, including my health and fitness products list.
- Click here to buy me a virtual cuppa
- Sign up to my mailing list
- Women can join my feminist Facebook group – the Nomipalony Freehouse

Disclaimer: This post contains affiliate links. If you purchase through an affiliate link you will not be charged any more for your purchase, but I will receive a small fee for referring you. As an Amazon Associate, I earn from qualifying purchases. For my full disclosure policy, please see my about page.
Please note this blog post was first published 26th February 2016 but was last refreshed February 2023.



This is so fantastic! And well done! 9 months ago I had an emergency section at 41+6 after 3 sweeps, induction + waters broken. The crazy thing is, now looking back, he just wasn’t ready. We used Natal Hypnotherapy and were so calm that if I had trusted myself more I think my son would have arrived when he was ready. When I was reading your story it was like reading my own – 3/5 engaged, slow contractions. I had my second sweep on the Sat, induction Mon, into check induction progress Tues and section on Wed. I didn’t want to go into hospital on the Tues but I done what I was told! Next time I will be having my home birth, and I can’t wait! Thanks for sharing this
Oh wow, yes our first births were very similar. It’s hard to trust your instincts when hospital policies are pressuring you to fit in with them but I really believe there is nothing more important than a mother’s instinct. I bet you have an awesome home birth next time. Join the groups I mention if you haven’t already as they are full of supportive, informed and like minded women. They helped me so much! Good luck on your journey.
I have LOVED reading this post and loved that you have so many photos from your birth too. All three of my births were very different but unlike you I LOVED my birthing pool and felt like it really took the pressure off.
That’s fab Samantha! I would still get a pool again if I was to do it again. I was just surprised that it wasn’t as helpful as I expected and that the tens machine was more helpful. I’m so pleased I got photos, I would have loved a birth photographer but already felt there were too many people in the room. I have a few videos too but they are pretty graphic!
Ah I love a home birth story, my midwife (who may have been one of yours too) was a home birther and very supportive of my plans to homebirth my second and third children it’s an amazing and wonderful feeling to be curled up with your family safely at home without any fuss
I didn’t know you home birthed too! That’s awesome. What were your midwives called? I had Sue and Allison. They were fab! Yeah I totally agree. Home sweet home!
Every time I read your story I cry, because I know how much you wanted this.
With Noah, while I was lucky to have a natural (unmedicated and no interventions) birth in a hospital, Ziva’s birth (at home) was a million times different (and healing) for me. The comfort of home and knowing your team supports you 100% makes the experience all that more rewarding.
I, like North East Family Fun, had a wonderful experience with the tub, but my birth with Ziva was less than 6 hours and my husband barely had time to fill the tub (we even ran out of hot water and my doula and he were bringing up boiling pots of water). I didn’t get into the tub until after my waters broke, and I literally sprinted upstairs, in between contractions, to get to the tub in time.
My absolute favorite part of the home birth was being able to hold her for 45 minutes. No one else really touched her (though my midwife did do some quick tests to make sure she was ok) and no one tried to take her away from me. Whereas with Noah I held him for less than a minute and then they whisked him away, after which my husband held him the entire time until we had him taken to the nursery, so we could get rest (24 hours of labor and being awake for over 28). I will forever regret not making my husband give Noah to me and that we made him go to the nursery alone for the first few hours of his life (it still makes me cry to this day, even now as I write this, the thought that he was all alone after just coming into the world).
Anyway, I digress, I’m still so thrilled you were able to heal from A’s birth, he’s such a wonderful little boy!!!!! I wish more women would opt to have their babies at home and realize just how amazing the experience can be.
You’re amazingly strong and I’m still so proud of you!!! You did it against all the odds.
Thanks so much Hannah! Your support and knowledge helped me do it. I hope you become a doula one day as I think you would be incredible at it. Try not best yourself up about Noah, you know better you do better and you are an amazing Mam. It’s easy to forget how tired you are in that moment, no one would blame you for self care after going through all that. Thanks for your comment. Xx
This is about the tenth time I’ve read your HBAC story and I love it every time! I’m 33 weeks at the mo with my second and am planning an HBAC but I’m starting to have a bit of a wobble. I’ve researched everything and have resource papers coming out of my ears, it’s just now I’m getting closer to the end I’m wondering if we’ve made the right decision. I’ve always known the minute risk of uterine rupture but the ‘what if’ is creeping in now. I just wondered if you’d ever had a wobble on your decision and if so how you dealt with it? P.S. I’m a slow cooker too, first bubba didn’t arrive until 42+4! Xx
Oh I’m so pleased you like the post Rachael. I think it’s really natural to have a wobble. I know that I did and my friends who had home births did too. For me I think it’s that everyone is constantly telling you how scary it is but of course there are so many risks with hospital births that no one ever mentions. It’s so biased. I’d just listen to your gut, follow whatever it tells you. There is nothing more powerful than a mother’s intuition! Good luck and do come back and let me know how you got on
Hi Nyomi! Just thought I’d let you know my little girl was born on Tuesday! A long latent phase and significant meconium after my waters went meant we made the decision to go in to hospital. 3hrs 21mins of active labour and only 7mins of pushing and Hope Enfys was in my arms! Even though we didn’t get the HBAC we planned the birth couldn’t have been more perfect. The staff at our hospital were so respectful of our choices (a lot of which went against hospital protocol) and never once did I feel like things were out of my control, a world away from my first little girl’s birth.
Reading your blog has been such a massive help all through my pregnancy xx
Oh that’s fantastic Rachael! Thanks so much for letting me know. I’m so pleased you got a VBAC and they were respectful of your choices. I’m so happy for you!! Xx
Well thus just made me bawl. We’ll done for going ahead with it and you certainly turned a traumatic first birth into a positive experience
Thank you! X